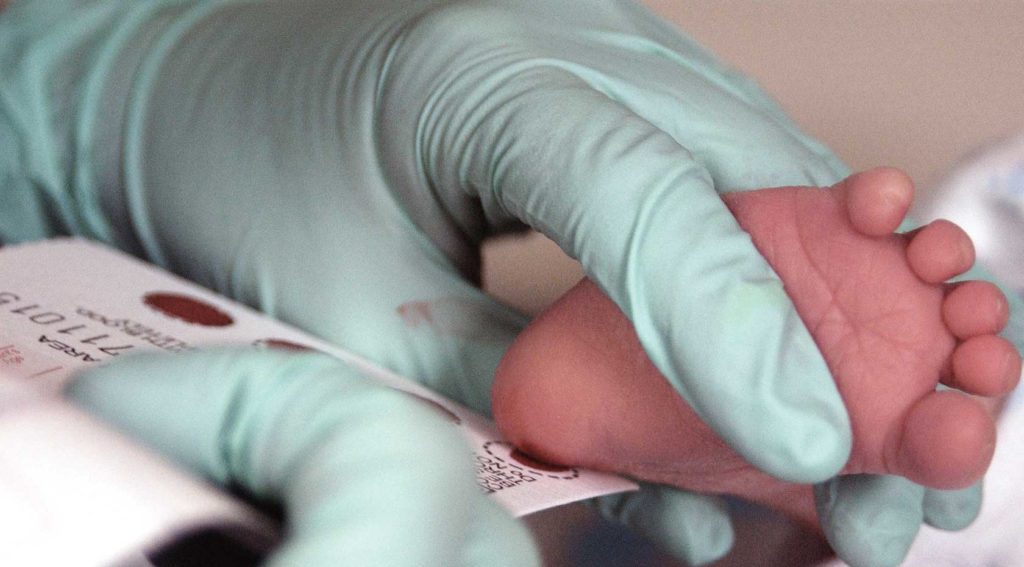
By 2006, universal newborn screening was in place in all 50 states, Puerto Rico and the U.S. Virgin Islands. Within 48 hours of birth a few drops of blood from the infant’s heel undergo tests for several disorders, including hearing loss and critical congenital heart defects.
The Massachusetts Department of Public Health mandates screening for 32 disorders. Tests are performed through the New England Newborn Screening Program at the University of Massachusetts Medical School in Worcester.
A misprint
A test called hemoglobin electrophoresis (e-lec-tro-for-ee-sis) measures a protein in the red blood cells called hemoglobin. This protein is essential to the body. It carries and dispenses oxygen, a source of energy to organs and tissues. Without it we cannot survive.
But in some newborns, the hemoglobin has a misprint. Just one gene goes awry, causing a change in the structure of the red blood cells. Generally, these cells are round and flexible and flow with ease through the network of arteries. Instead, they are sticky and sickle shaped. They can get stuck in the blood vessels and block the flow of blood, causing severe pain, infections and a myriad of complications. Their shelf life is limited. Normal red blood cells survive for 120 days, the sickled cells only 10 to 20, increasing the risk of anemia.
This is called sickle cell disease (SCD).
SCD is a genetic disorder and is inherited from both parents. It’s nothing you catch like the flu or measles. The exact number of people living with SCD in the U.S. is unknown, according to the Centers for Disease Control and Prevention (CDC). The best estimate is 100,000 Americans. Minorities are hard hit. The disease affects one out of every 365 African American births. It is also more frequent in Hispanics and people from the Caribbean, Saudi Arabia, India and Mediterranean countries, such as Greece, Turkey and Italy.
Some newborns inherit the defective hemoglobin from only one parent. This is called sickle cell trait (SCT). Generally, this form of the disease is silent. People often don’t know they are afflicted since it typically does not share the same complications as SCD. Yet, SCT is more common, afflicting about one in 13 African Americans.
That’s the problem. Those with SCT are carriers and can unknowingly pass the disease on to their children. Adults can be tested for SCT, but some prefer not to know. They fear the stigma or being labeled, explained Dr. David Sykes, a hematologist at Massachusetts General Hospital. Yet, if two people with SCT bear children, with each pregnancy there is a 25% chance of producing a child with SCD. Testing or genetic counseling may be of interest to couples planning a family.
Complications
In SCD no organ is spared. Blood vessels are like highways in the body. They transport blood everywhere. The disease can damage the eyes, liver, lungs, bones and joints and heart. It can lead to leg ulcers, multiple organ failure and increased infections due to damage of the spleen. At least 30% develop chronic kidney failure.
The first attack can occur as young as five months, often in the form of hand and foot syndrome, characterized by painful, swollen hands and feet. Infants and children can even suffer strokes.
But the hallmark of SCD is the pain crisis called vaso-occlusion that results from the acute lack of oxygen to tissues and organs. Pain is the leading cause of emergency room visits and hospitalizations for those afflicted, according to a Statistical Brief from the Agency for Healthcare Research and Quality.
Yet, SCD is unpredictable. Some people experience problems infrequently and feel overall quite well, while others are hospitalized multiple times each year.

A step forward
At one time many kids with SCD never survived to adolescence. But in 1998, hydroxyurea was approved for adults, then children in 2017. Hydroxyurea helps the body make more good hemoglobin. It also makes red blood cells bigger and helps them stay rounder and more flexible. Newer medications have been developed more recently to reduce the frequency of pain crises or improve anemia.
The impact of hydroxyurea has been dramatic. From 1979 to 2017, SCD-related death rates among Black children younger than five years of age declined 158%, according to the CDC. During the same period the median age at death increased from 28 years to 43 years. However, this is still a much younger age than for people without SCD.
Day by day
Still there is a closely followed regimen to follow. Key is plain tap water. People with SCD are advised to drink at least eight glasses of water every day to decrease the risk of a crisis. Daily vitamin B12 and folic acid helps prevent severe anemia. Children younger than five years should take oral penicillin twice a day. Blood transfusions may be warranted to help treat anemia and prevent stroke. Appropriate attire for the weather is necessary for extreme temperatures, both hot and cold. A yearly eye exam screens for retinopathy. Vaccinations protect against pneumonia, meningitis and influenza.
At times an emergency
Even with fastidious monitoring, however, a serious complication can develop. Fever greater than 100.5°F is a tell-tale sign, according to Sykes. Difficulty breathing and chest pain are red flags. Dedicated SCD infusion centers are preferable over emergency rooms. These are outpatient centers where staff are well acquainted with the patients’ needs. People with SCD often require enormous amounts of opioids to quell pain crises, but some providers who are not familiar with the treatment of SCD patients are reluctant to prescribe them. “Patients wind up being undertreated,” said Sykes.
Possible cure
A bone marrow transplant can cure some people with SCD. The procedure replaces the bone marrow of the patient with healthy blood-forming cells from a donor. It can be a precarious procedure and requires heavy doses of chemotherapy. Although a cure, it is difficult to find donors, and is performed in only certain hospitals.
Gene editing takes another approach. It’s designed to correct the mutation in hemoglobin, thus eliminating the need for a donor. The studies are currently in clinical trials.
Hidden scars
The emotional impact of the disease cannot be overlooked. A report published by the Centers for Medicare & Medicaid Services examined the most prevalent chronic conditions for people with SCD covered by Medicare. People with SCD are often covered under Medicare because of disabilities and kidney failure.
In 2016, the two most prevalent chronic conditions were pain and hypertension, closely followed by depression and anxiety disorder. The conditions were most common between the ages of 31 and 64. This is understandable. SCD often gets worse with age. “It leaves small scars over time,” explained Sykes. “Even if you don’t notice, it does cumulative damage over the years. It adds more pain on top of the organ damage.”
Supporting hand
Studies show that strong and long-term family support are important factors to improve life expectancy and quality of life in SCD patients. More people are surviving to their sixth or seventh decade. Sykes agrees and adds the professional team to the list. “Having a strong and trusting relationship with the medical team is important to long-term health.”
Symptoms and complications
Abnormal hemoglobin and blocked blood vessels cause a myriad of complications in people with sickle cell disease.
• Anemia
• Hand-foot syndrome — severe pain and swelling in hands and feet; often the first symptom of SCD in babies
• Pain crises
• Infections, particularly pneumonia and meningitis
• Acute chest syndrome — severe infection of the lungs
• Splenic sequestration — enlargement of spleen caused by trapped red blood cells
• Vision problems
• Pulmonary hypertension
• Delayed growth and puberty
• Gallstones
• Stroke
• Leg ulcers
• Kidney disease
• Pregnancy difficulties
• Priapism — painful erections in males
Common Triggers
• Change in temperature, usually cold
• Strenuous exercise
• Lack of water
• Stress
• High altitudes
• Infections
• Smoking
• Alcohol
• Fatigue










