Report shows breast cancer survival rates worst among Black women
Age, body mass index, tumor subtype among factors, MGH researchers say
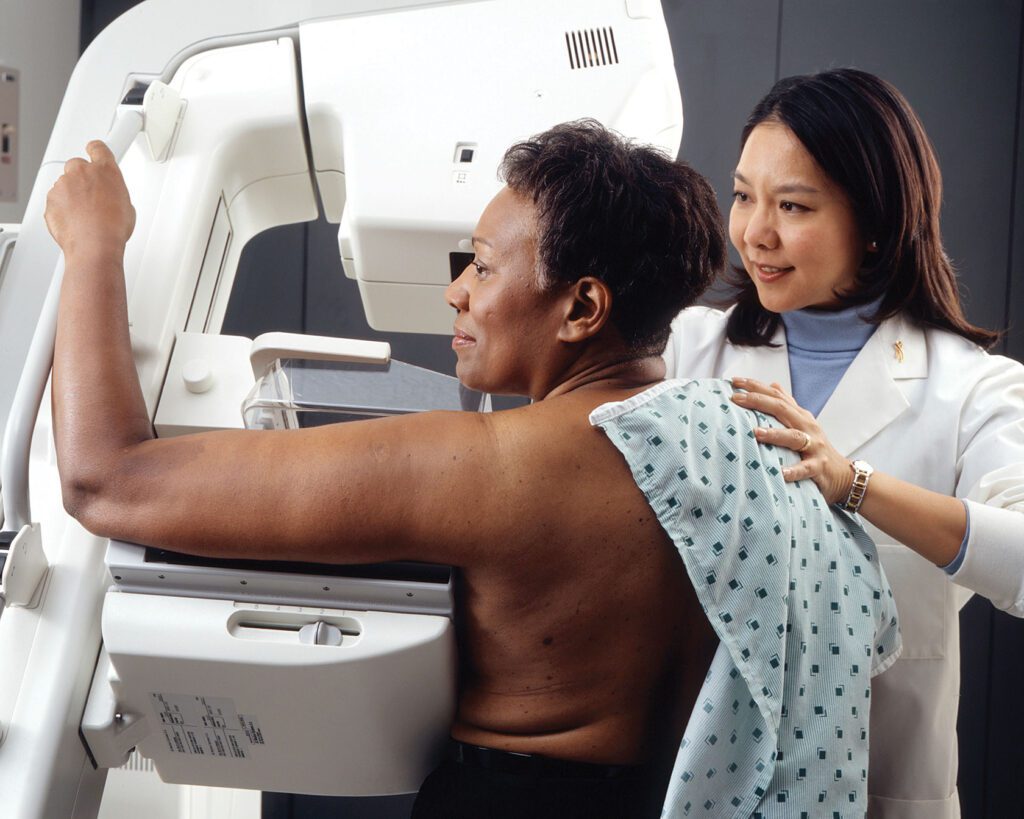
Black patients had worse breast cancer outcomes than their white counterparts, according to researchers at Mass General Cancer Center who also noted other factors that contribute to survival rates.
The researchers, who recently published their findings in JAMA — Journal of the American Medical Association — found that age, body mass index and tumor subtype were also critical factors.
“It’s critical to evaluate interventions for equitable improvement in survivorship,” said Erica Warner, one of the researchers in the study, in a statement to the Banner.
The researchers analyzed nearly 9,500 participants, including nearly 900 Black patients, with available survival data and race and ethnicity data from four chemotherapy trials. They identified people in subgroups, defined by tumor subtype, age and/or body mass index, that may drive racial and ethnic disparities in survival.
Researchers noted that for several decades, non-Hispanic Black women have had substantially higher breast cancer mortality rates than non-Hispanic white women. They pointed out data from the Surveillance, Epidemiology, and End Results program showing that between 2015 and 2019, Black women had 41% higher breast cancer mortality compared with white women despite a 4% lower incidence of breast cancer.
“The emergence and subsequent widening of this disparity over the past 40 years suggests that potentially modifiable and time-varying factors contribute,’’ the report said. “Such disparities are also known to exist among Hispanic women, although there is a relative dearth of literature studying this important population.”
The researchers noted that while lack of quality and timely initial treatment are important contributors, prospective study of breast cancer survival in patients receiving standardized adjuvant therapy, as in the clinical trial setting, can facilitate identification of other factors.
The researchers said the data show that survival differences exist even within clinical trial participants receiving similar initial care. They noted that multiple factors, including age, body mass index and tumor subtype, contribute to disparities in the mortality rate but their role remains unclear, they said.
The study said that young breast cancer survivors, who typically have longer life expectancies if cured, are at increased risk of developing toxic cardiac effects, depression and secondary cancers.
It also said disparities in treatment of these conditions as well as other non-cancer related conditions may be driving the racial and ethnic disparities in younger patients.
Reaction to the study has been varied among medical experts and breast cancer survivors.
The survivors said patients should advocate more for themselves, while the experts say that healthcare officials should provide more access to mammogram screenings, prioritize the care of traditionally marginalized patients and determine the best ways to serve them.
“We (need to) wrap our arms around our Black women (and) patients in breast cancer care, take a hard look at ourselves, our systems, our assumptions, and decide that we are going to do something better,” said Dr. Naomi Ko, an oncologist at Boston Medical Center. “We are going to change to improve the lives of these women who deserve to get optimal care.”
Karen Burns White, a deputy associate director at Dana-Farber/Harvard Cancer Center, said that the findings on Black women’s higher mortality rates are a major concern, but they are not new. White said she has since developed relationships with community partners to discuss various health and wellness topics.
“I approach community partners … in the space of health and wellness … to say, what is it that you believe your membership wants to know more about, and so at times, that could be areas impacting diabetes or areas impacting hypertension,” Burns White said. “It could be around looking at a variety of risk factors … engaging (the) community in a way where they’re setting the agenda.”
Michelle S. Williams, an associate professor at George Mason University, said women should feel empowered to seek other care if they are not getting what they deserve from their primary care doctor.
“Sometimes physicians don’t get it right,” Williams said. “And we have to be comfortable saying ‘You know, I want to go to another provider and get a second opinion.’”
C. Virginia Fields, president and chief executive officer of Black Health, recommends that patients who normally do not advocate for themselves consider bringing an outspoken family member or friend to their doctor’s appointment with them.
“Many (patients) think that the doctor has all the answers, and you can’t question them,” said Fields, who is also a breast cancer survivor.
She also urges patients to write down their symptoms and questions so “they can read from it or they can share it with the doctor,” she said.
Nekia Clark, a breast cancer survivor and co-chair of the Boston Breast Cancer Equity Coalition at the Ellie Fund, said the report’s findings are “awful” but not surprising. It’s one of the reasons, she said, that she began engaging in her current work.
“It doesn’t have to be that way,” Clark said. “It’s disturbing to hear (about the report’s findings) when breast cancer can be curable, if you get it at an early stage.”
Jani Raynor, a Roxbury breast cancer survivor, said patients should become more empowered and advocate for themselves. Raynor, who has a family history of breast cancer, recounted her own cancer journey.
She said she had found a lump in her breast in 2020 during the pandemic, which made it difficult for her to get a mammogram. At the time she had just had a baby. She was diagnosed with stage 3 C breast cancer in February 2022, she said.
“I had not had a mammogram prior to this (diagnosis),” Raynor said. “The lump was a substantial size. I could feel it very easily.”
She said that since she was unable to see her primary care physician, she ended up calling a cancer imaging center to make an appointment.
“A lot of times, because we have dense breasts, historically (as) women of color, it’s hard to find lumps. Mine was substantial, so it was quite easy to recognize,” Raynor said. “Cancer can … disguise itself. So it’s really important to know your breasts, examine your breasts — to look at how they look.”
After undergoing chemotherapy, a mastectomy and proton radiation therapy, Raynor said her active treatment ended in November 2022. She is now taking chemotherapy medication, she said.






